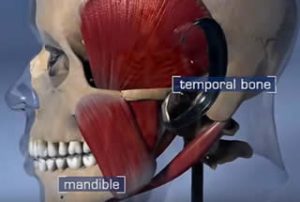
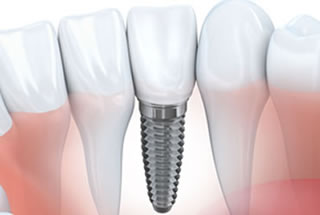
Even though regular checkups and proper dental hygiene greatly decrease the need for root canal treatment, the fact remains that it is one of the most common procedures performed by dentists today. What are some of the most common reasons you might need this dental solution?
Decay:
The primary cause for root canal procedures is decay that has entered the tooth pulp chamber and progressed to the point of causing infection or abscesses. Pain and tooth sensitivity often accompanies severe decay. Root canal treatment is the best way to avoid tooth extraction and restore oral health.
Trauma:
If a tooth endures strong force such as from a sports injury, car accident or fall, the trauma can damage the tooth so badly that root canal treatment is needed. Even if trauma isn’t completely evident at first, a severed nerve to the tooth can cause it to die over time.
Genetics:
Traits of teeth like their strength are passed along through genes. Some people inherit soft teeth that are more prone to decay, making it difficult to avoid decay even with diligent oral hygiene.
Tooth fracture:
A tooth can be fractured through chewing hard foods or ice, teeth grinding or clenching, or habits like nail biting. Even hairline fractures may allow bacteria to enter the tooth’s pulp and cause infections. Once the bacteria takes hold, root canal treatment may become necessary.
Deep cavity:
Deep cavities within teeth can allow infections to thrive, eventually causing the tooth to become inflamed or die. A deep cavity isn’t necessarily painful, so patients may not even realize they have an infection. Regular dental checkups help catch cavities early, before they are able to become so deep and serious.
Previous dental work:
Extensive or repeated dental work can cause trauma to teeth nerves and associated inflammation, making root canal therapy an important solution.
Do you live in Toronto or the surrounding area? Our team is ready to help you achieve your smile goals. Schedule your appointment today.
A toothache can make everything seem terrible. Your mouth hurts, your head aches, you can’t eat what you want, you can’t sleep comfortably – in general, you feel awful! Your tooth pain may be a result of decay that has caused an infection in your tooth pulp, calling for root canal therapy.
What does that mean exactly? When the inside of your tooth or the pulp becomes infected, it causes the tooth to deteriorate and cause pain and sensitivity. Action is needed to eliminate the infection and protect the tooth from worse damage. Root canal treatment is the best solution because the damaged pulp is removed and the inside of the tooth is thoroughly cleaned and restored.
To accomplish a root canal procedure, your dentist will drill a small hole in your tooth to access the pulp and expertly remove it. Once the area is cleaned and disinfected, your tooth will be filled with a special material and sealed for protection. Finally, a dental crown is usually placed on top to complete the root canal procedure. You are left with a fully repaired and protected tooth.
What benefits does root canal treatment provide?
- Pain is eliminated with the repair of your tooth and removal of infection.
- Your ability to chew and bite foods will return to normal.
- You will no longer experience tooth sensitivity to hot or cold items.
- The damaged tooth will be restored so that it looks natural in your smile.
- Your other teeth won’t have excessive wear to make up for the damaged tooth.
With the advances in dentistry making root canal therapy faster and less painful, your procedure may be completed in as little as one trip to the dentist. Once the process is complete, you can expect your fully restored tooth to last as long as the rest of your teeth.
Are dental issues holding you back? Take control of your oral health by booking an appointment with our experienced team at our Toronto dental office.
A toothache can make your life miserable. It may involve terrible tooth pain as well as headaches, sleeplessness, and difficulty eating. A trip to the dentist’s office is a must if you want relief. An examination might reveal that you need root canal treatment to save your tooth and eliminate your symptoms.
Severe tooth decay, a faulty crown, repeated tooth procedures or trauma are common causes of tooth damage. These issues can also lead to infection of your tooth’s pulp, which is on the inside of your tooth. Also called endodontic therapy, root canal treatment focuses on getting rid of the damaged tooth pulp. If infection is present, it is also removed. The root canal is thoroughly cleaned and disinfected, and then the area is filled with a special material called gutta-percha. Finally, the tooth is typically restored with a dental crown to provide maximum protection from future damage.
Some of the benefits you can expect from root canal treatment include chewing with normal biting force and sensation, maintaining natural tooth appearance, protecting other teeth from excessive wear, and avoiding a troublesome gap in the smile. In as little as one or two appointments, these benefits can be achieved without a great deal of discomfort. Innovations in technology have made the experience of root canal treatment usually no more painful or difficult than simply getting a dental filling. Once root canal treatment is complete, the tooth can last a lifetime with regular checkups and proper oral hygiene.
Do you live in Toronto or the surrounding area? Our team is ready to help you achieve your smile goals. Schedule your appointment today.
Having tooth pain or problems can be one of the most uncomfortable experiences possible. It is hard to ignore because it makes your whole quality of life worse. When infection or decay reaches the inner parts of your tooth, it can cause many miserable symptoms. Often the key is getting root canal treatment to save your tooth and alleviate your symptoms. Here are some warning signs that indicate you might need this type of treatment.
Severe pain:
Although not always present, severe pain sometimes occurs with a tooth that needs root canal therapy. It may be sharp, intense pain or a dull ache that won’t subside. If you experience tooth pain that is severe or lasts for several days, see your dentist for an evaluation. If root canal treatment is necessary, any pain you may have will likely disappear after a successful procedure.
Sensitivity to hot or cold:
Discomfort when consuming hot or cold items is another sign of a problem. Mild sensitivity is usually not a big deal, but actual pain when your tooth hits these temperatures may mean the tooth is in an advanced stage of trouble.
Gum tenderness or inflammation:
Swelling or tenderness is often associated with infection, although it doesn’t always mean infection is present. Your dentist can determine the seriousness of the issues and whether root canal treatment is advised. Watch for tenderness, swelling, or even a lump in the affected area.
Darkened tooth:
Discoloration is a sign that the nerves of a tooth are damaged. The tooth may become gray, black or dark yellow. Tooth discoloration is also related to trauma, damaged fillings or severe decay, so visiting your dentist for a checkup is recommended.
Gum boils:
If lesions similar to a pimple form in the gum tissues, it is called a gum boil. It is usually an accumulation of pus, which can be linked to infection. The boil may be larger or smaller at certain times, depending on the activity of the infection in your mouth. It will feel tender and can cause swelling in the area, and you may notice a bad taste in your mouth.
If you have symptoms such as these, see your dentist to learn if root canal treatment is the solution.
Do you live in Toronto or the surrounding area? Our team is ready to help you achieve your smile goals. Schedule your appointment today.
If root canal treatment has been recommended for you, you’re probably a little nervous. Maybe you’re a LOT nervous, but if you’re thinking about putting off your treatment, don’t. If you need root canal therapy, the underlying conditions that necessitate it will not go away left untreated. In fact, they’ll just get worse and worse over time, causing you more pain and discomfort and potentially leading to more serious complications.
If you don’t treat the infection in your tooth, it will spread. Beginning at your tooth’s roots, it will travel to your jawbone and eventually to your healthy teeth. Your entire jawbone can be put at risk. By treating your infection promptly with root canal therapy, your mouth can be free of infection and you will begin the process of healing.
Serious diseases like heart disease and diabetes have been directly linked to gum disease. During pregnancy, many problems including low birth weight and premature birth can occur as a direct result of infection and bacteria in the mouth. Several types of cancers have all been shown to have a link to poor overall oral health. The mouth is truly the pathway for everything that goes into the body, and if it’s providing a steady stream of bacteria and infection to be spread throughout your body, it’s extremely problematic.
Don’t worry about pain following your procedure. Root canal therapies are meant to relieve pain, not cause it. You’ll be surprised how much better you’ll feel after your mouth is infection-free.
If you ignore your infected tooth for long enough, it may either fall out on its own or need to be extracted. Missing teeth come with a long list of oral issues, including difficulties with bite alignment and speech only corrected with some kind of dental restoration.
Don’t wait to have your root canal treatment. Don’t open yourself up to the myriad of consequences that could result from postponing treatment.
Do not let another day go by without taking care of your dental needs. Request an appointment now at our Toronto dental office!
If you suspect you have an infected tooth, you might wonder if root canal treatment might be in your future. Do you have another option? Yes! One such alternative has been in existence for decades, but has only recently come to be more effective due to advancements in materials. This process is called pulp capping.
Pulp capping can help patients whose root infections have not yet reached the tooth’s nerve. Root infections begin when bacteria enters the pulp of the tooth through a crack or a large cavity. In a standard root canal procedure, the pulp and nerve of the tooth is hollowed out, cleaned and sealed, typically with a crown restoration.
With pulp capping, the nerve is preserved and the tooth is often repaired with a filling instead of a crown. Pulp capping allows the dentist to clean and protect the pulp, defending it from infection with medicine. With a successful pulp cap, the dentin of the tooth begins to regrow over the pulp cap. Advancements in the sealants used during these types of procedures has allowed for a greater percentage of success.
If you have a toothache, it’s important to see your dentist immediately. Pulp capping has a narrow window in which it can be performed. If your tooth is too infected, the pulp and nerve of your tooth may already be infected, and it’s too late for pulp capping to be effective.
A pulp cap is a far less invasive procedure than a root canal treatment or a tooth extraction, and there is less recovery time and tooth sensitivity following the treatment.
If you suspect you may have a tooth in trouble, talk to your dentist now. You might be able to save yourself a root canal treatment.
Take the first step towards optimal oral hygiene. Reserve your dental appointment at our Toronto dental office now and experience personalized care.

 E-Mail Us
E-Mail Us  416-595-5490
416-595-5490